Creating a Sensory Diet at Home
How to use items you already have at home for your child’s sensory diet
One of our very favorite ways of addressing hot clinical topics is through a Q&A format. Learn from Occupational Therapist, Ellen Snyder, as she uncovers some of the most commonly asked questions from our parents and caregivers when it comes to establishing a sensory diet. Most, if not all of these items, can be found already laying around your house or can be purchased locally. You may also decide to conveniently take items on the go!
Q: What is a sensory diet?
A: A sensory diet is a set or sequence of activities that engage multiple sensory systems. This can calm the child and help focus attention.
Q: What sensory systems do sensory diets target?
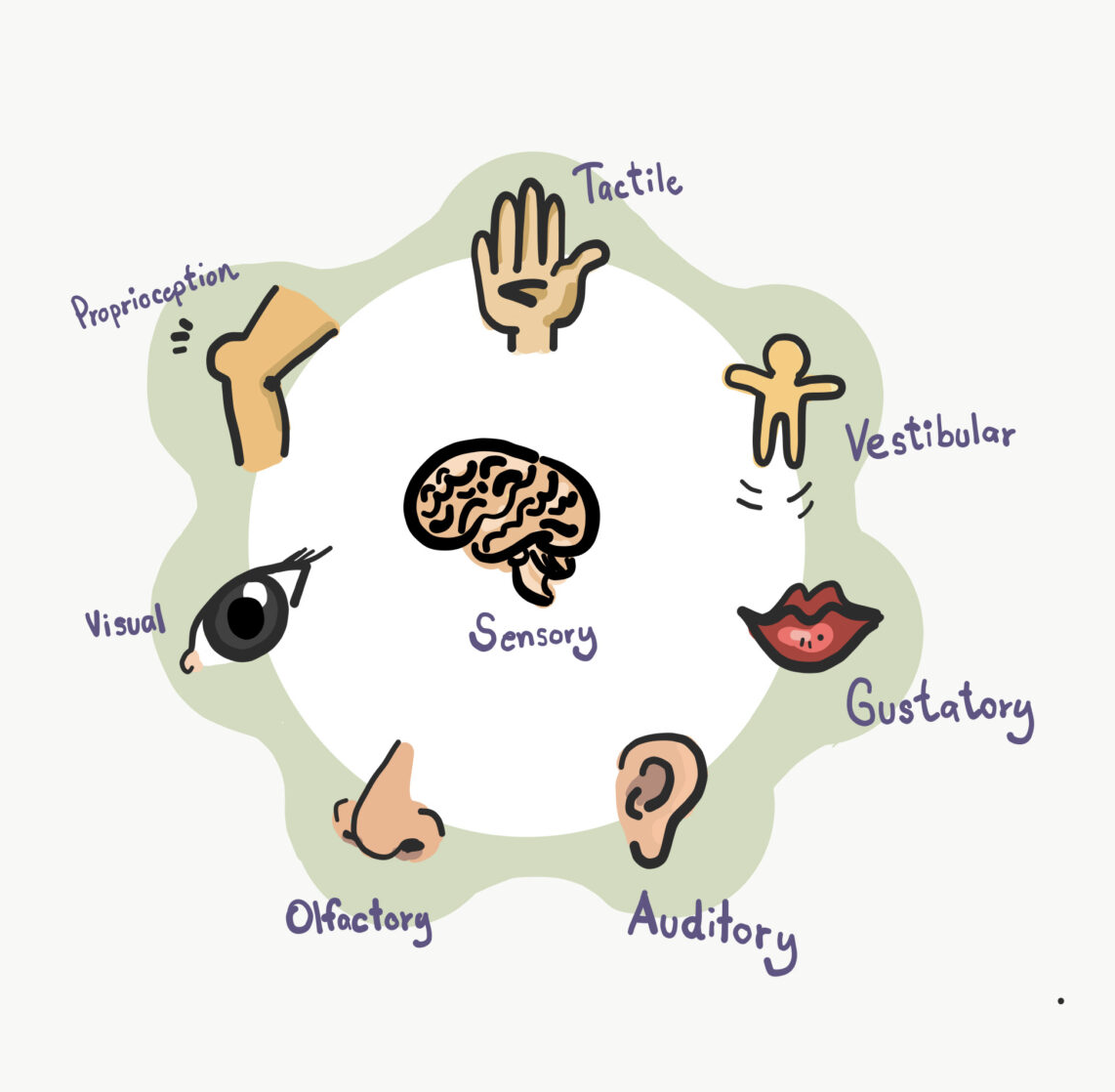
A: The focus of the sensory diet will depend on your child's momentary needs. We have seven sensory systems (I know school only teaches us we have five, but there are two very important invisible ones).
Auditory/sound
Visual/sight
Gustatory/taste
Olfactory/smell
Tactile/touch
Vestibular/balance: allows the body to be balanced, know how fast and in what direction the head is moving, and allows the body to adjust to any changes in the head or the environment. This system is located in the inner ear.
Proprioceptive: allows the body to know where it is in space either at rest or while moving without the use of vision and to be able to make postural adjustments. This system is located throughout the body in the joints, tendons, and muscles.
Q: Who needs a sensory diet?
A: Everyone has a sensory system and can benefit from specific sensory input, however certain children may need a little extra support to get their sensory needs met. One way to think about this is with a cup analogy. If you think of each system as having an individual cup, the cup needs to be filled to meet his/her sensory needs. Until these sensory needs are met, it can be difficult for your child to attend to activities, listen to and follow directions, and keep his/her body safe. As each child and his/her sensory system is unique, the “size of the cup” will vary. For example, a child sensitive to sound has a “small auditory system cup” and it doesn’t take much sound to fill his cup. Another child might have a “large tactile system cup” and needs a lot of tactile play to fill his cup before his sensory system is satisfied. A few of the diagnoses that benefit from a sensory diet include: Attention Deficit Hyperactivity Disorder (ADHD), Autism Spectrum Disorder (ASD), and Sensory Processing Disorder (SPD).
Q: Can I give too much sensory input to my child?
A: The only system that doesn’t become over-sensitive is the Proprioceptive system (deep pressure). All other systems can become overwhelmed and lead to increased dysfunction. Think, of becoming dizzy after spinning, or over-sensitive to loud sounds or bright lights when in a busy place.
Q: What can I do to help regulate my child after too much sensory stimulation?
A: Input to the proprioceptive system can help the nervous system become regulated after too much of another type of sensory input. Deep squeezes on arms, hands, legs, feet, and gentle deep pressure on the head, pushing, pulling, or lifting an item with weight or resistance.
Decreasing as much other sensory stimulation as possible, such as moving to a quiet room or smaller space, dimming lights, and reducing sound can help your child become calmer and allow his/her nervous system to not have to work as hard to filter out the external sensory stimulation.
Q: What is a time-effective way to provide the sensory stimulation my child needs during the day?
A: The best way to help your child get the sensory stimulation his/her body and nervous system need is to work it into their daily routine. When a child wakes up, provide deep squeezes to the head, arms, trunk, and legs (tactile, proprioceptive). Moving to different areas in the house, encourage your child to move like an animal (vestibular, proprioceptive, tactile, visual systems). Use of visual picture schedules for daily routine (visual system). Depending on your child’s needs allow for quiet or preferred music during breakfast (auditory, olfactory, gustatory). Carrying a backpack to the car and riding with it on their lap (proprioceptive).
You can absolutely work with your child’s therapist to help solve how to integrate these activities into daily life.
Q: Why does my child not become calm after 10 minutes of jumping on the trampoline?
A: For some children, although they appear to crave constant movement, such as jumping, swinging, being upside down, and running around, their nervous system has a hard time knowing what to do with certain types of sensory stimulation. Think of a filing cabinet with no organizational system (their brain/nervous system) and the file (sensory input) doesn’t have a clear place to be filed.
Structured sensory-based activities will be the most effective and help organize your child’s nervous system. Movement with a purpose or a goal will help your child from becoming dysregulated from the type of input he/she is wanting. Some examples are jumping to a song and doing a freeze dance, running to gather specific items and bringing them to a specific location, swinging and giving high fives or reaching for a puzzle piece, crawling over pillows with a straw to blow a pom-pom on the floor, or locating hidden objects in a bean bin.
It’s easy to think of a sensory system in isolation, however as we exist in the world we are constantly experiencing sensory input from the clothes on our body, to the smells and sights, and sounds we experience. Because of this fact, it is so important to encourage our kids to play using many different sensory systems. This will naturally help them integrate their sensory systems and get the input they need.
Q: What are some typical household items to use for a sensory diet?
A:
Sheets for swinging and sliding around on the floor.
Painters tape to make a balance beam course on the floor.
Dried beans, pasta, rice, and lentils for sensory boxes.
Playdoh - can make homemade with flour, oil, water, salt, and cream of tartar
Slime - there are many recipes to make at home
Empty bottle for I-spy bottle with small items and rice
Pillows or couch cushions for crashes, crawling over or building forts
Spray water bottles
Boxes for drawing, cutting, or creating small spaces
Twinkle lights
Scented lotion
Handheld massagers
Electric toothbrushes
Chewing gum
Blowing bubbles with a straw, dish soap, and water
Tongs
Puzzles
Headphones
Speaker for music
Learn more about Occupational Therapy services at Marshall Pediatric Therapy and how your family can benefit, here.
)